Anal Cancer is a malignancy that arises in the tissues of the anus, most commonly from the lining cells of the anal canal. It can develop as anal squamous cell carcinoma, adenocarcinoma, or other rarer histologic types, with squamous cell carcinoma being the most frequent. Several factors can contribute to risk, including infection with human papillomavirus (HPV), particularly high-risk HPV types, and a history of anal or cervical dysplasia. Immunosuppression is also associated with higher risk, such as in people living with human immunodeficiency virus (HIV) or those taking immunosuppressive medications. Other contributing factors may include smoking and chronic inflammatory conditions affecting the anorectal region.
Anal cancer commonly presents with symptoms related to local growth and irritation. People may notice bleeding from the anus, pain or discomfort in the anal area, itching, or a persistent sensation of a lump. Some individuals develop changes in bowel habits, including constipation or a feeling of incomplete evacuation, though these are not specific. On examination, clinicians may find an ulcerated or raised lesion, and in some cases enlarged lymph nodes in the groin can occur due to spread through lymphatic pathways. Because symptoms can overlap with benign anorectal conditions, diagnosis typically relies on clinical evaluation and tissue testing.
Historically, anal cancer was less common than many other gastrointestinal cancers, but its incidence has been influenced by changes in HPV prevalence and survival patterns in immunocompromised populations. Medical literature has long recognized the strong association between HPV and anal squamous cell carcinoma, supporting the role of viral-driven cellular changes in carcinogenesis. The terminology and classification of anal tumors have evolved with advances in pathology, including clearer distinctions between squamous, glandular, and neuroendocrine tumors. Epidemiologic studies have helped characterize risk groups, including people with HPV-related disease and those with impaired immune function. Today, conventional medicine describes anal cancer in terms of tumor type, stage, and extent of spread, which are key for understanding prognosis and clinical behavior.
Note: This description was generated by AI and may contain inaccurate information.
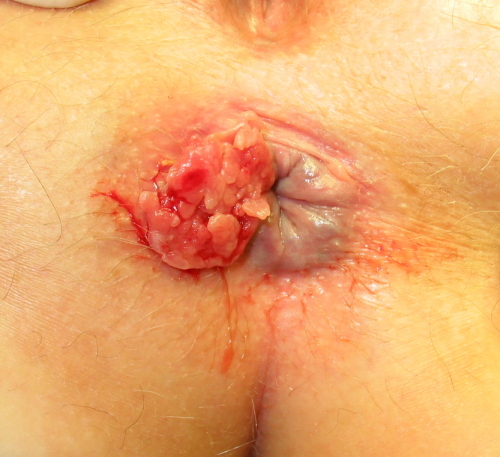
Original Image Producer: Dr. K.-H. Günther, Klinikum Main Spessart, Lohr am Main. Credit: Dr. K.-H. Günther, Klinikum Main Spessart, Lohr am Main. License: CC BY 3.0. Link to Source: https://commons.wikimedia.org/wiki/File:Squamous_cell_carcinoma_of_anal_rim_01.jpg .
Rectal Mass Shrinks After Three Months of MMS1 & MMS2
I had discovered CD when arguing with someone on Twitter about the use of HCQ curing COVID. Someone posted the Quantum Leap video below my argument. I watched it and ordered it right away.
My husband and I took it for a month to prove its safeness as my sister’s father-in-law was just diagnosed with cancer and I wanted to help. Sadly, he decided not to take the CD.
Then my mother started feeling ill. Because she knew it was safe and felt comfortable, she started taking it right away. Then a week later she saw her doctor and they found a mass 7 cm large in her rectum and the doctors told her she would need a colostomy bag.
After about 3 months of MMS1 & MMS2 her mass shrunk to be superficial. They were able to remove it and could never find the cancer cells. Though it was in the muscle so the doctors kept saying it had to be cancerous.
I know God led me to this. Thank you, thank you for fighting for truth.

